Dr Mecherl Lim
An Intuitive Medical Practitioner in Alternative Medicine (MD) (MA), Naturopath (ND), Holistic Kinesiology (HK), and Functional Medicine (FM)
Food Allergy occurs when the body has chemical reaction to eating a particular food & drink. The symptoms for mild to moderate food allergy or intolerance may sometimes be similar, but food intolerance does not involve the immune system and does not cause severe allergic reactions (Anaphylaxis)
A Food Allergy occurs when the immune system reacts to harmless food. Learn to read food labels so you can avoid foods that cause allergic reactions.
Food Allergy & Food Intolerance
Symptoms of food intolerance occasionally resemble those of food allergy so food intolerance is commonly confused with food allergy. Food intolerance does not involve the immune system and does not cause severe allergic reactions (know as anaphylaxis). Food intolerance also does not show on allergy testing. Food intolerance can be a difficult concept to understand and is poorly understood by doctors as well. Sometimes, substances within foods can increase the frequency and severity of migraine, headaches, rashes (such as hives) or stomach upset such as irritable bowel.
Professional diagnosis and confirmation of allergies is important. In Australia, about one in 10 infants, one in 20 children up to 5 years of age, and two in 100 adults have food allergies.
Food Allergies has been Increasing
Allergies in general are on the increase worldwide and food allergies have also become more common, particularly PEANUT ALLERGY in preschool children. About 60 per cent of allergies appear during the first year of life. Cow’s milk allergy is one of the most common in early childhood. Most children grow out of it before they start school.
Inherited Allergy
Children who have one family member with allergy disease (including asthma or eczema) have a 20-40 percent higher risk of developing allergy. If there are two or more family members with allergy disease, the risk increase to 50 to 80 percent.
Most of the time, children with food allergy do not have parents with food allergy. However, if a family has one child with food allergy, their brothers or sisters are at a slightly higher risk of having food allergy themselves, although that risk is still relatively low.
Allergy is an Immune Response
Allergies are an overreaction of the body’s immune system to a protein. These proteins may be from foods, pollens, house dust, animal hair or mould. They are call ALLERGENS. The word allergy means that the immune system has responded to a harmless substance as if it was toxic.
Food Intolerance is a Chemical Reaction
- Food Intolerance is a chemical reaction that some people have after eating or drinking some foods: It is not an immune response.
- Food Intolerance also does not show on allergy testing.
- Food Intolerance can be a difficult concept for doctors as well. Sometimes substances within foods can increase the frequent severity of migraine headaches, rashes (such as Hives) or stomach upset.
- Food Intolerance has been associated with Asthma, Chronic Fatigue and Irritable Bowel Syndrome (IBS).
- Professional diagnosis and confirmation of allergies is important in Australia, about one in 10 infants, or in 20 children up to 5 years of age and two in 100 adults have food allergies.
Therapy
The preferable approach to the nutritional management of immunological food reactions or food hypersensitivities consists of dietary avoidance and the treatment of symptoms resulting from inadvertent exposure. Nutritional supplements are needed when major food groups are being avoided. This will ensure the optimum nutritional intakes are maintained. Digestive enzymes example: Dr MH zyame should be taken by individuals who seems to be sensitive to many foods. Bicarbonate of soda , Dr MH Proflora A, taken one hour after meals can improve symptoms. By improving digestion the allergenic load may be destroyed or digested more thoroughly.
Visit : www.drmecherlherbs.com
Email : drmecherherbs@gmail.com
FACEBOOK : drmecherlherbs for further enquiries.



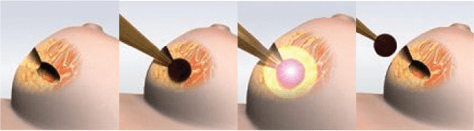 Breast Cancer is the most common cancer amongst women in the world. Incidence of breast cancer is increasing and the lifetime risk of developing breast cancer in Malaysia is one in 15 women. In developed countries, the lifetime risk of developing breast cancer in women is as high as 1 in 8 women. With more awareness and screening for breast cancer, women are detecting breast cancers earlier, which are smaller and have better survival outcome.
Breast Cancer is the most common cancer amongst women in the world. Incidence of breast cancer is increasing and the lifetime risk of developing breast cancer in Malaysia is one in 15 women. In developed countries, the lifetime risk of developing breast cancer in women is as high as 1 in 8 women. With more awareness and screening for breast cancer, women are detecting breast cancers earlier, which are smaller and have better survival outcome.


